
The Interconnected Road to Organ Preservation Innovation
How Collaboration Across Stakeholders Leads to Better Patient Outcomes

Guest Author:
Perry Turner
Managing Director, Commercial + Clinical Operations
Organ Recovery Systems
When the average person envisions organ donation or transplantation, they might imagine a straightforward or “simple” process. In this scenario, a surgeon swoops in quickly, retrieves an organ, and whisks it off to a patient in need. While not necessarily untrue, the reality is that every safe and successful transplant relies on so much more: the entirety of a complex ecosystem working in sync.
What this “simple” scenario fails to account for are the advocacy groups, the organ procurement organizations (OPOs), clinicians, researchers, and private-sector partners all playing distinct yet synergistic roles to ensure patient safety and a successful transplant. Successful outcomes require coordination that can stretch across hundreds of miles, multiple forms of transportation, and involve varying types of medical professionals. Everyone involved carries the responsibility to align their efforts and execute their role seamlessly to honor the gift of donation and the generosity of donor families, every time.
It Starts on the Front Line
The donation and transplant community would look vastly different today if no one dared to challenge the status quo. Static cold storage (SCS), keeping organs on ice, is one of the most widely used and clinically accepted methods for graft preservation, which means keeping organs viable outside the body between recovery and transplant. SCS involves drastically lowering the temperature of the organ by storing it in a special ice mixture to prevent the breakdown of the organ. This method is favored due to its simplicity and relatively low cost. However, it is not without its own limitations, including time constraints, ischemia-reperfusion injury, lack of viability metrics, and increased risk with medically complex organs. [1]
Organ preservation has evolved from simple static cold storage to today’s machine perfusion technologies, which circulate fluid through the organ to help preserve function and provide additional information to clinicians before transplant. These innovations emerged directly from clinicians advocating for safer, more reliable solutions. As a result, advances like machine perfusion have provided clinicians with additional techniques to evaluate and preserve organs, especially during kidney transplants (Figure 1). This evolution and community shift has not just improved graft survival, it has fundamentally changed how donation and transplant professionals assess and support donors.
Figure 1
Proportion of Kidneys Transplanted with Machine Perfusion, Mar. 2017 to Feb. 2026
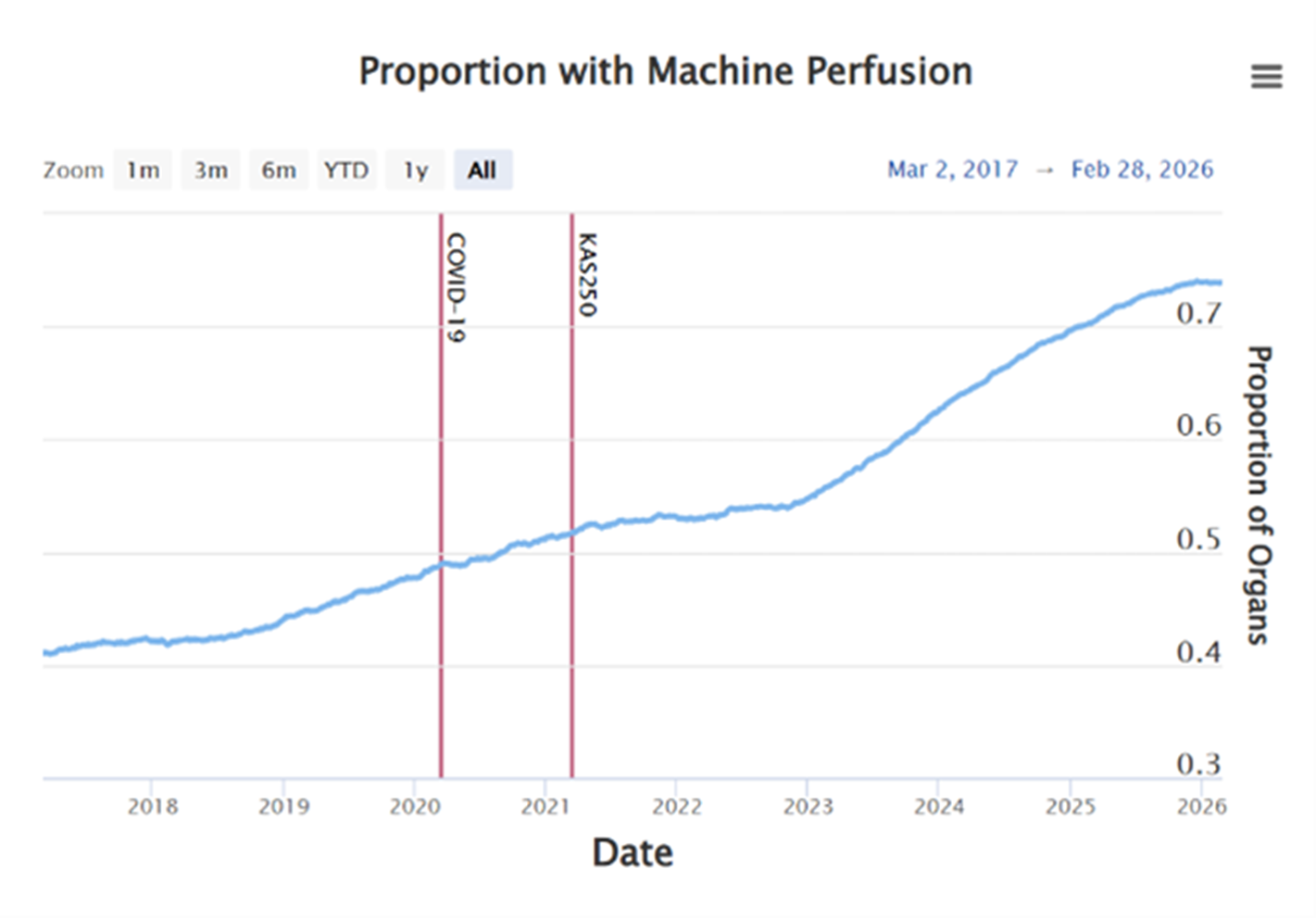
Source: The data is from the Scientific Registry of Transplant Recipients, SRTR.org
Historically, most donated kidneys came from Donation after Brain Death (DBD) donors, meaning that death is declared based on the irreversible cessation of all brain function, including the brain stem. However, with machine perfusion enabling safer, more informed evaluations of organs outside the body, there has been a dramatic shift towards accepting more organs that would not have been deemed “viable” in the past. Today, the donor landscape has reached a 50/50 split between DBD and Donation after Circulatory Death (DCD) donors (Figure 2), reflecting how these technologies have expanded viability and confidence in decision making for organs once considered higher risk.
Figure 2
Proportion of Kidney Donations that are DCD, Mar. 2017 to Feb. 2026
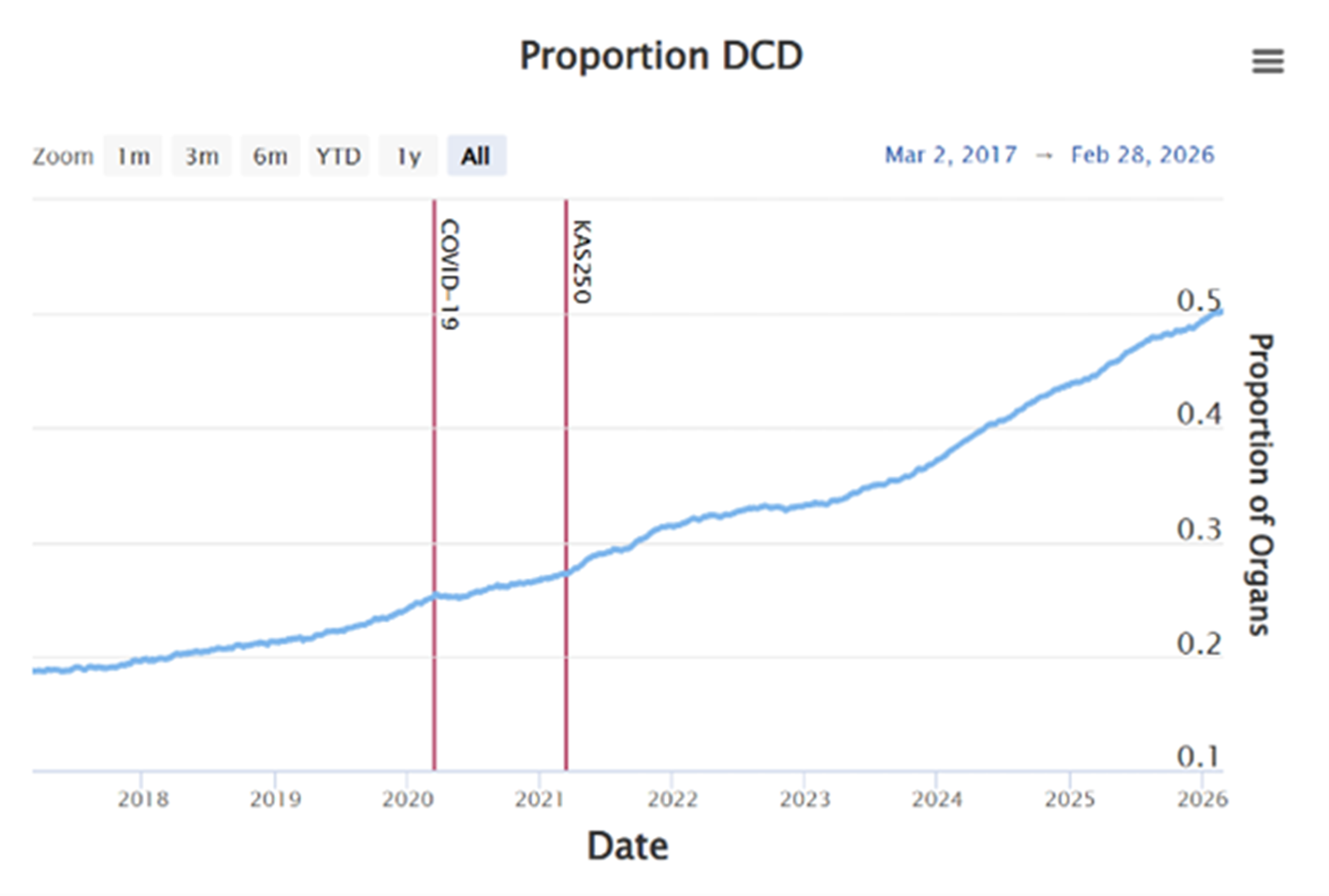
Source: The data is from the Scientific Registry of Transplant Recipients, SRTR.org
Frontline healthcare workers and transplant surgeons play a critical role in identifying areas for improvement in patient care and donation. These insights have always been a starting point for innovation, while public-sector organizations and OPOs rely on those innovations to fill resource gaps and support their mission-driven work. One cannot succeed without the other. A balanced ecosystem consisting of academics, OPOs, industry partners, nonprofits, and medical professionals brings a mix of scientific research, community support, patient support, technological advances all with the singular goal of better patient care and outcomes. When these perspectives are aligned, the system is better positioned to serve patients and families.
Collaborative partnerships across the donation and transplant community help support resource-constrained allies or colleagues, allowing consistent improvements across the system. The ripple effect of everyone operating at their best and participating fully in this framework is felt by all, but most importantly the patients, as this model accelerates the pace of new technologies, solutions, and methods in real-world practices.
Understanding Our Role in the System
Industry partners, like Organ Recovery Systems, play an important role in supporting the donation and transplant system by developing tools and technologies that assist clinicians and OPOs. These efforts rely on the individuals and organizations doing the difficult and important work of facilitating, performing, and supporting organ donation and transplantation. Feedback from clinicians and OPOs helps identify challenges in processes or areas for improvement to ensure successful donation and transplant outcomes. This collaboration informs organizations to innovate and manufacture transplant technologies.
Machine perfusion itself is the result of decades of progress, with early prototypes in the 1990’s resulting in today’s portable, data-rich devices. What started as a concept to reduce ischemic injury, cellular damage to the organ as a result of loss of blood and oxygen flow, has grown into a sophisticated portfolio of medical technology with features prioritizing extended preservation times, real-time viability metrics, and better patient outcomes.
New and emerging features in today’s technologies are continuing this trajectory, and OPO leaders have expressed optimism in the direction the technology is heading. Remote monitoring dashboards allow OPOs and surgeons to review the same organ data simultaneously, improving shared decision-making. Extended-window perfusion means clinicians have more time to coordinate complex logistics across longer distances. Portability has always been a high priority, with devices outfitted for Federal Aviation Administration (FAA) compliance for commercial flights, helping ensure organs can be transported safely and efficiently.

Pictured: A Delta pilot smiles with an ORS LifePort Kidney Transporter ahead of a commercial flight during a recent transplant journey.
As the needs of modern transplantation grow, the community requires more reliable and scientifically proven technology that is safe. Hypothermic machine perfusion, backed with years of clinical data [2] and improved long-term results for recipients, is becoming a new standard of care. In addition, as scientific evidence continues to support machine perfusion, modifications to hypothermic machine perfusion, such as oxygen supplementation, have shown promising results and are becoming more widely adopted. [3]
All Voices, One Mission
To the surgeons, transplant coordinators, OPOs, and nonprofits: please ask for more from your industry partners, and know that we want to help. The future and direction of the donation and transplant community relies on those who are on the ground, so keep advocating for devices and technologies that complement real-world applications and scenarios. It is well understood that a collaborative effort will be needed to meet the growing demand and aspiration to increase utilization of donor organs and save more lives. [4]
For industry members and private sector organizations: innovate and create with these real-world experiences in mind. Cater designs as a complement to alleviate pain points and inefficiencies. And beyond the physical contributions of these organizations, continue to lend resources and time to causes and efforts that advance the community forward. Volunteering, participating in joint initiatives, and amplifying the stories of donor families, recipients and patient advocates are ways the community can stretch its collective impact into something tangible far beyond operating rooms and hospitals.
In a field defined by urgency, complexity, and human generosity, it relies on a symphony of coordinated efforts across disciplines for one core mission. This complexity is manageable when every voice in the ecosystem is heard, making the impossible achievable. The interconnected road to better outcomes does not exist without the whole community participating. The next era of donation and transplantation will be built in the same way the community has evolved to this point, with collaboration, innovation, barrier-breaking, and always with patients and families at the center.
About the Author:
With more than 20 years in solid organ transplantation, medical device, and sales and management leadership experience, Perry Turner leads the commercial and clinical operations for Organ Recovery Systems. This includes oversight of the organization’s clinical and technical advisors, strategic account managers, and the two LifePort Preservation Centers. To learn more about Organ Recovery Systems, visit https://www.organ-recovery.com/.
Organ Recovery Systems is an AOPO Gold Level Industry Partner.
